Contact us

Why Is Stereotactic Radiosurgery Often Called Gamma Knife?
Why Is Stereotactic Radiosurgery Often Called Gamma Knife?
One of the most fascinating aspects of stereotactic radiosurgery is that despite being called a surgery, it is able to carefully target and destroy tumours without the need to open up a part of the body and cut them out.
Sometimes, when researching stereotactic radiosurgery (SRS) ahead of booking an appointment, you may come across the term Gamma Knife, which is sometimes used as an interchangeable term to describe a type of non-surgical targeted radiotherapy.
This can cause confusion, but it is easier to consider Gamma Knife as a particular type of targeted stereotactic radiosurgery aimed at treating brain tumours and lesions.
The reason for the confusion is a matter of chronology; the Gamma Knife method was one of the earliest successful forms of SRS, first conceived by Lars Leksell in 1949 as a way to treat small lesions on the brain that would be too dangerous to manage with conventional surgery.
It took until 1968 for the Gamma Knife itself to be first implemented at the Karolinska Institute, but once it was it became the defining type of SRS for many years to the point that a lot of people would use the term Gamma Knife as a genericised trademark for all types of targeted radiotherapy.
However, as the concept of SRS evolved and became capable of treating many other parts of the body besides the brain, calling all treatments in that category Gamma Knife radiosurgery became increasingly inaccurate.
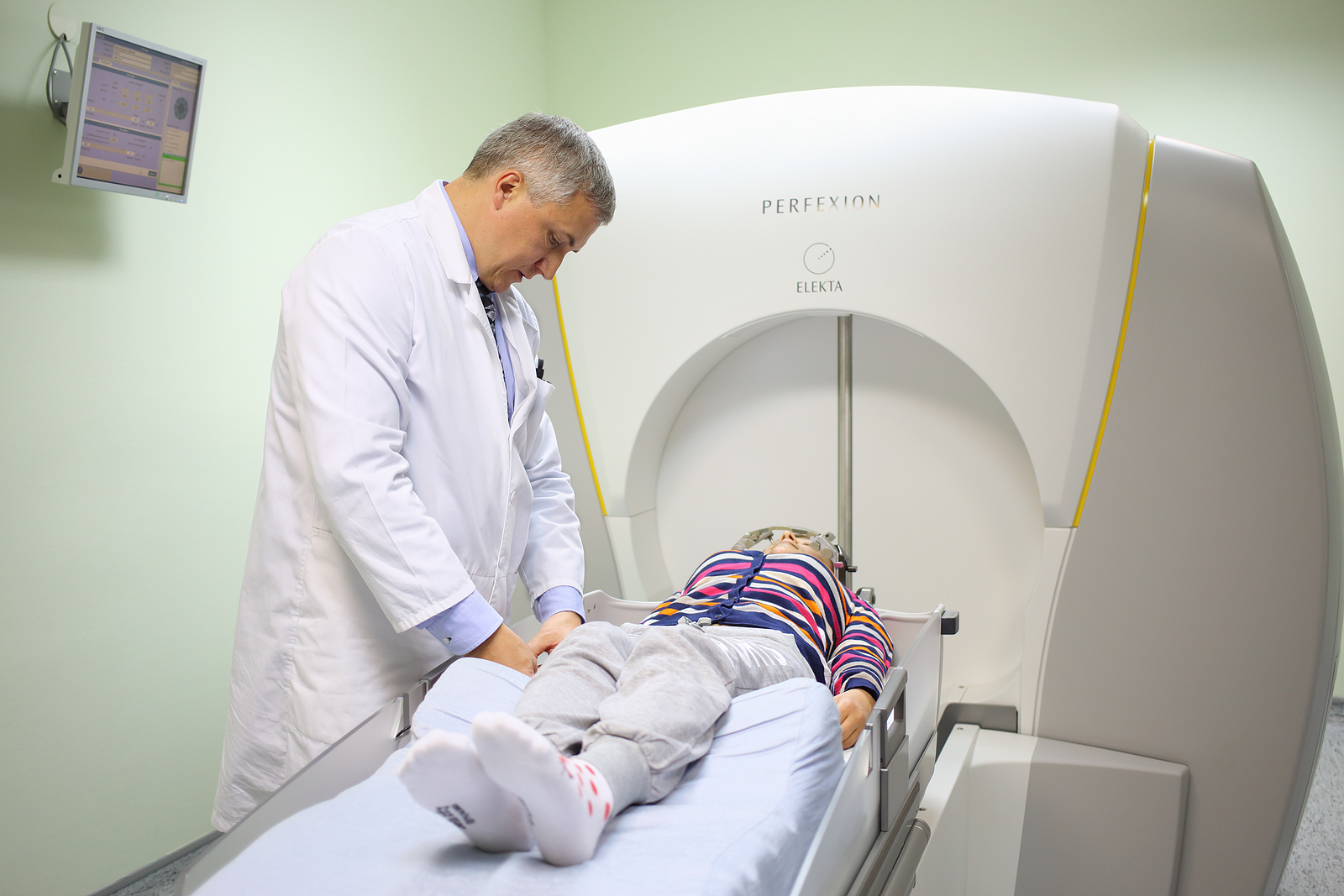
With alternative treatments available that can treat a wide variety of tumours all over the body, many radiologists prefer to use the more general term stereotactic radiosurgery unless specifically referring to the Gamma Knife technique, including a headframe, helmet and array of radioactive beams.
Where this becomes most confusing is with the CyberKnife system, a versatile SRS system inspired by the Gamma Knife technique but able to treat tumours in the throat, liver, pancreas, brain and prostate.
Ultimately, there is a wide range of SRS treatments, and Gamma Knife is one of many.