Contact us

Radiation Therapy
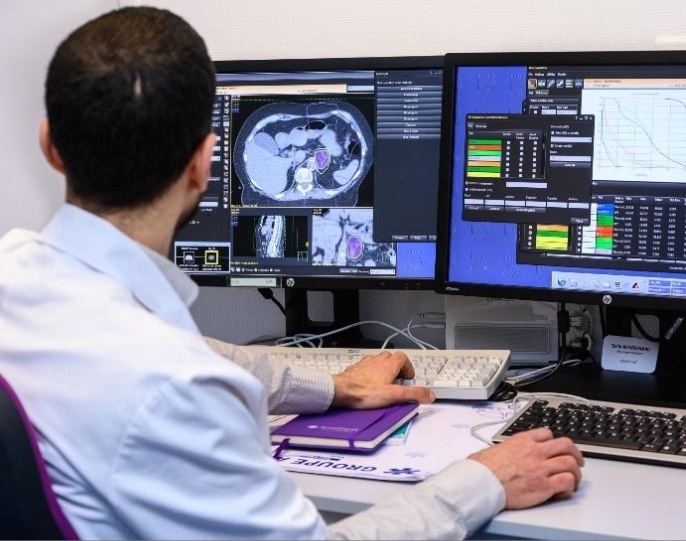
Radiation therapy (also called radiotherapy) works by aiming a high dose of radiation towards a patient’s tumour, which damages cells’ DNA. Cancer cells whose DNA is damaged beyond repair stop replicating and die. The body then breaks them down and removes them.
Depending on the pathology, it takes days or weeks of treatment before cancer cells are damaged enough for cancer cells to die. Cancer cells keep dying for weeks or months after radiation therapy ends.
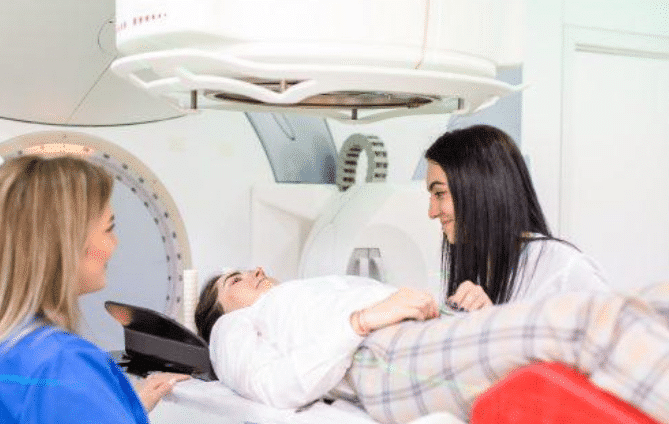
Two main types of radiation therapies:
external beam therapy and internal radiation therapy
(also called brachytherapy)
The type of radiation therapy used depends on many factors, including type of cancer, size of the tumour, its location within the body, patient medical condition, his/her medical history, etc.
External beam radiation

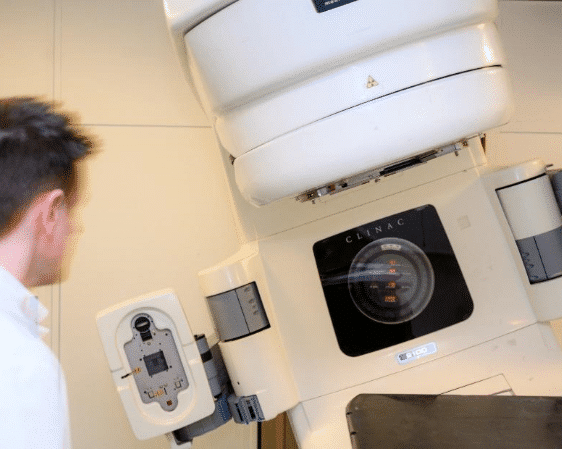
This treatment method delivers one or several beams of high-energy x-rays to a patient’s tumour. Beams are generated outside the patient (usually by a linear accelerator – also called Linac) and are targeted at the tumour location.
The machine is large and can move around the patient during treatment, sending radiation to a part of the body from many directions in order to concentrate them on the cancer. Advanced
radiotherapy techniques aim to maximise the radiation dose that the tumour gets while minimising the dose received by healthy tissues surrounding the tumour.
The duration of radiation therapy depends on the type of cancer being treated and whether the goal of radiation therapy is to treat the cancer or ease symptoms.
Usually external beam radiation is given to patients across a number of sessions that are spread out over time (several weeks), allowing healthy cells to recover between radiation therapy
sessions.
Advanced radiotherapy techniques include IMRT, VMAT and stereotaxic radiosurgery
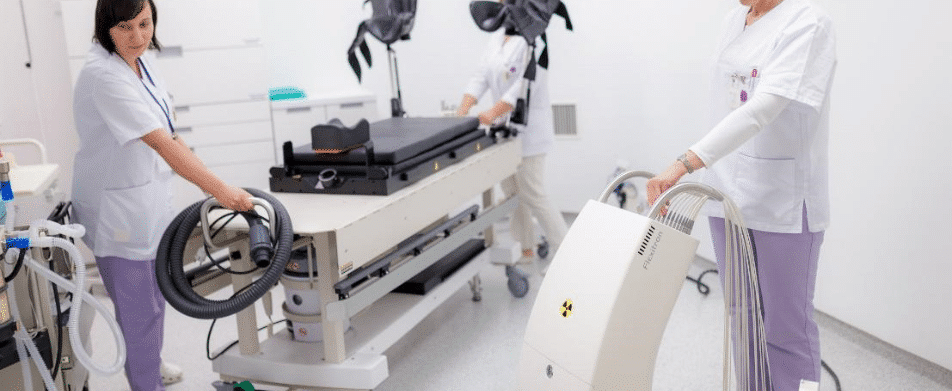
Internal radiation therapy
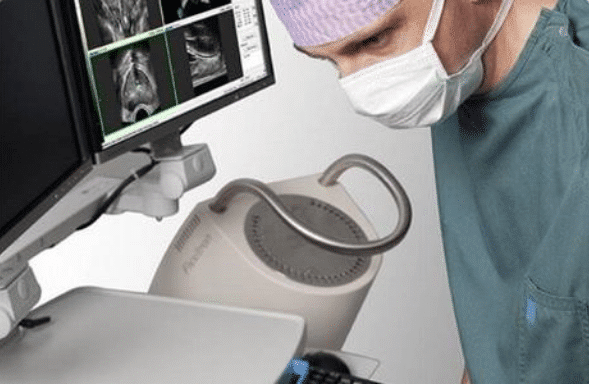
Internal radiation therapy is a treatment in which a source of radiation is placed inside the patient on a temporary or permanent basis.
In brachytherapy, seeds, ribbons, or capsules that contain the radioactive source are placed in or near the tumour. Brachytherapy enables to treat a tumour with very high dose of localised radiation whilst reducing the probability of unnecessary damage to surrounding healthy tissues.
While external beam radiation therapy is used to treat many types of cancer, brachytherapy is most often used to treat cancers of the head and neck, breast, cervix, prostate, and eye.
Advanced radiotherapy techniques

At Amethyst Radiotherapy centres, we use the most advanced radiotherapy techniques, such as IMRT, VMAT or stereotaxic radiosurgery.
Advanced medical imaging combined with state-of-the-art radiotherapy equipment allow to deliver a high dose of radiation, to the tumour, while preserving healthy tissues surrounding the tumour and minimizing the adverse effects of treatment.
Intensity-modulated radiotherapy or IMRT
Intensity Modulated Radio Therapy is a conformational radiotherapy technique in which the dose of irradiation delivered by each beam is modulated to administer higher dose to the tumour while minimizing exposure to irradiation of surrounding areas.
The linear accelerator – or LINAC – has a device called multi leaf collimator (MLC), which consists of thin movable tungsten leaves that can block part of the radiation field. As the leaves can be moved independently, the radiation can be modelled so that its intensity is maximum at the tumour, and minimal in the surrounding areas.
With IMRT treatment, the dose of radiation is concentrated on the volume of the cancerous tumor, thus sparing healthy tissues and organs and reducing the patient’s risk of developing long-term complications.
Volumetric Modulated Arc Therapy or VMAT
VMAT – also called Arc Therapy or Rapid Arc radiotherapy – is an IMRT technique which is highly accurate and precise.
With VMAT, radiation beam is being delivered in an arc that moves around the tumour and the beam shape and radiation dose automatically change as it moves.
Treatment planning with VMAT is much more accurate and healthy tissues receive only a very limited fraction of the radiation. This innovative technique, combined with image-guided irradiation processes, ensures high-precision processing.
The average time to exposure to radiation for this type of treatment is reduced to a few minutes. In addition, the exposure to radiation is reduced to a few minutes. Treatment with VMAT is therefore not only faster, but also more accurate, with minimal side effects.

Stereotactic radiotherapy
Stereotactic radiotherapy (also called stereotactic radiosurgery) is a non-surgical radiation therapy used to deliver precisely targeted radiation to small tumours, located in the brain or in the body.
Stereotactic radiotherapy involves the delivery of higher doses of radiation to the tumour (typically equivalent to one week of classical external irradiation), throughout a smaller number of treatment sessions (also called fractions).
The performance of stereotactic radiotherapy is demonstrated in a wide variety of cancers, used to treat both primary cancer (where the cancer started such as the lung or the prostate), or locations where a cancer may have spread (secondary cancers or metastases).
As stereotactic radiotherapy requires millimetric accuracy, it requires Image Guided Radiation Therapy (IGRT) – which uses medical imaging to confirm the location of the tumour before and during the radiation treatment.
It also requires patient-specific immobilisation devices – such as head and neck masks – to ensure perfect immobility of the targeted body part.