Contact us

How Intensity Modulated Radiation Therapy Can Be Used
How Intensity Modulated Radiation Therapy Can Be Used
The use of radiotherapy is not a particularly new technique, being used as a cancer treatment from the turn of the 20th Century, just a few years after Nobel Prize-winning German physics professor Wilhelm Conrad Roentgen discovered X-rays and their capability not just to see inside the human body, but also treat malignant cells.
Radiation has the quality of being able to alter DNA, which means it can prevent cancer cells from dividing and growing. At the very least it will slow the progress of a cancer, but in some cases, it can kill off a tumour entirely.
However, it was soon established that this cancer treatment came with a major downside as the radiation could also be harmful to neighbouring tissue and bring a range of unpleasant side effects. Just as it can damage the DNA of cancer cells, it can do the same to healthy ones.
Maximising Doses While Minimising Side-Effects
It is because of this that the quest has been underway for a long time to find ways of being ever more precise in the delivery of radiation to areas of the body affected by cancer, in order to ensure the maximum blast of treatment to take down cancerous cells while minimising exposure elsewhere.
This became possible from the 1930s onwards, as the arrival of the ionising chamber in 1932 meant that for the first time, it was possible to measure the radiation dose accurately. This made it possible to calibrate machinery to control how much radiation was in each dose and thus avoid – or at least reduce – some of the worst side effects.
Many techniques have been developed down the years, such as the use of gamma knives for brain tumour surgery, but another that may not be familiar to many people is intensity modulated radiotherapy, or IMRT.
What Is IMRT?
IMRT uses linear accelerators to deliver the radiation and has been designed to be very precise in the doses it gives and where it directs them. It is used against tumours, either to prevent the whole tumour from growing or to target specific areas of it.
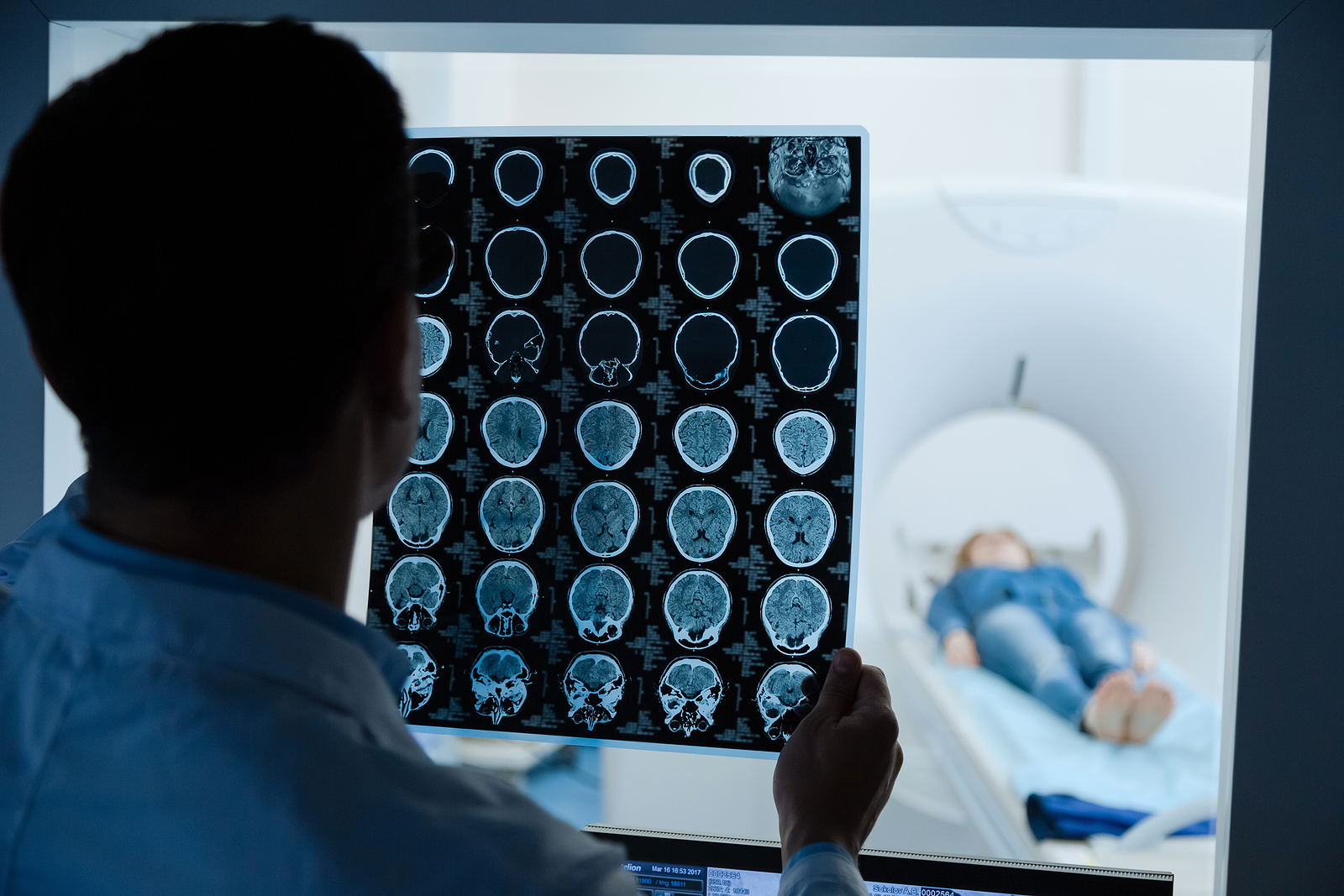
The intensity modulation part is connected to the fact that the system, which is computer-operated, uses 3D imaging of the tumour (either 3-D computed tomography or magnetic resonance) to navigate exactly what its shape is and where the radiation should be delivered.
Rather than a single beam aimed in a specific direction, a session using this technique will involve multiple beams of different intensities aimed at various parts of a tumour. The use of the 3D scans will enable the computer to calculate exactly what doses should be delivered to each area. This makes the treatment highly individualised.
As a result, there will be some areas that get a very high dose and others a lower one, as this enables an optimal amount of radiation to be used to blast the tumour where it will be most effective while doing the least damage to the surrounding non-cancerous tissue.
The great benefit of this is that it brings effective treatment with minimised toxicity. The only negative – and it is a price worth paying – is that the complexity of the treatment means the sessions will last for longer. That is a worthwhile trade-off when you face fewer side effects that would otherwise blight or prevent normal activities on non-treatment days.
Is It Right For You?
Indeed, with any cancer treatment, a consideration your oncologist will take into account will be quality of life. This is most obviously a consideration when a patient is at a point where their life can no longer be saved and it may be best to enjoy their remaining time as much as they can instead of undergoing more gruelling treatment.
For those who have been diagnosed at an early enough stage for the treatment to have a strong chance of being effective in limiting or even beating off cancer, the question is about balancing the essential requirement that the treatment be effective with the impact of the side effects on the patient.
If your condition is such that IMRT may provide the best option or one of them, your radiation oncologist will discuss this with you, helping draw up a personalised plan for your care based on the computer analysis of your 3D scan and, of course, seeking your consent to proceed. If it isn’t the right thing for you,
Various other specialists will be involved in your treatment, with a therapy nurse carrying out regular patient assessments to establish how the treatment is going and how well you are handling it. They will look for any adverse reactions as well as help you to deal with your symptoms.
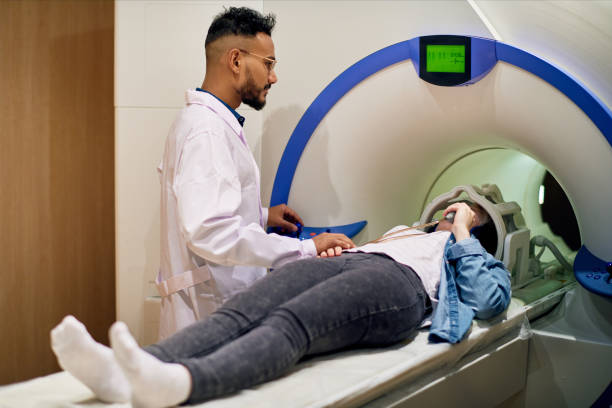
Treatment lasts between 15 minutes and an hour and while each patient is alone inside the machine, which is about the size of a car, they will be closely monitored from the outside. The patient will not feel anything, but will hear sound and occasionally detect a slight smell from the electronic equipment.
Treatment can take place on up to five days a week over a period of up to eight weeks and side-effects, while kept to a minimum, can still be significant and include localised hair loss, tummy trouble, urinary issues and localised soreness and swelling. Other skin problems like dryness and itching can occasionally occur.
How IMRT Began
IMRT is not as new a method of treatment as some might think. It was conceived in the 1960s when it was understood that three-dimensional targeting of tumours with variable radiation doses could produce more optimal results, but it was not until the 1980s and 1990s that the necessary computer capacity for the algorithms became available.
The first commercially available IMRT delivery system was the NOMOS Peacock System, which used a device known as a dynamic multivane intensity-modulating collimator.
Further systems have been developed in the 30 years since, providing ever more accurate calibration and efficient use of the radiation to deliver precisely the dose needed.
This means if you are under consideration for such a treatment, you can be assured the technology is very modern, yet uses well-established techniques based on very sound theories.